Dr. Kou-I Lin(right)and doctoral student Ming-Feng Chiang(left)
Dr. Kou-I Lin(right)and doctoral student Ming-Feng Chiang(left)
Blimp-1 is a transcriptional repressor, that is, a protein which can inhibit the expression of genes; it has been demonstrated to be a significant player in the immune system. In Dr. Kuo-I Lin’s 2012 study, she has identified that post-translational modification of Blimp-1 by SUMOylation acts as a crucial step to coordinate gene expressions when producing antibody-secreting plasma cells.
Led by Dr. Lin, the doctoral student Ming-Feng Chiang wanted to know if Blimp-1 plays any immunological role in keratinocytes, that is, the skin cells, which is the most visible protection system of our body.
As a matter of fact, they have not only found the answer positive, but also identified the existence of Blimp-1 in the skin cells links to the behaviors of certain immune cells attracted to epidermis, and the lack of Blimp-1 could be the cause of certain human skin inflammatory diseases. The study has been published in the PNAS Journal in Aprilthis year. As a very first one that reports the anti-inflammatory role for Blimp1 in the adult epidermis, the result drew quite attention to the Immunology world, and, separate briefings were reported in Nature Reviews Immunology in May as well as in the June edition of Nature Immunology.
All too often, the skin to us is so natural that we tend to think of it only as a protective barrier of our body that prevents outside intrusions. As a matter of fact, our skin not only creates a wall of protection, it has its own immune mechanism as well. When we have a cut or infection, an alert will be made to the skin immune system to activate all sorts of immune cells to start their duties to confront germs or other types of stress from outside.
Normally, when the skin damage is healed, the immune cells will be turned off to their original dormant state and wait for the next alarm. However, there are times that the skin immune responses go haywire, and the combat mission turned uncontrollable. As a result, annoying skin rashes, or more worse, eczema, may happen.
Immune system in our body is acting like the defense department of a nation. It has the built-in intelligence which knows what kind of guards to call for a mission, at what time and what location. The only catch is, when there is a slight variation to its original functional design, the protection system may appear as a rebellion that initiates confrontations inside our own body.
So, Lin’s team wants to know if Blimp-1 is also acting as a crucial regulator in the epidermal immune system. They first obtained skin specimens from Department of Dermatology of National Taiwan University Hospital. Their analysis showed a reduced amount of Blimp-1 in about 50% eczema samples that showed thickened layers of skin. Well, will the reduced Blimp-1 be a cause or a result of skin inflammation? Or, maybe it is just a coincidence?
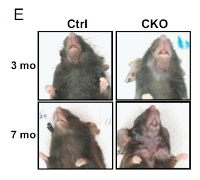 In order to pursue the study, the team first designed a way to genetically modify adult mice whose Blimp-1 is deleted from skin cells but remains in other cells. Three months after the Blimp-1 gene deletion, hairs around their necks started to fall, and by the time of the seventh month, ulcers started to develop on their skins. By double checking the neck skin, prior to the ulcers, the outer skin layers of Blimp-1 lacking mice were thickened, and signs of other immune cells were detected.
In order to pursue the study, the team first designed a way to genetically modify adult mice whose Blimp-1 is deleted from skin cells but remains in other cells. Three months after the Blimp-1 gene deletion, hairs around their necks started to fall, and by the time of the seventh month, ulcers started to develop on their skins. By double checking the neck skin, prior to the ulcers, the outer skin layers of Blimp-1 lacking mice were thickened, and signs of other immune cells were detected.
To further investigate what the immune cells were activated; also, why the inflammation started from the neck, the team worked with Dr. Fu-Tong Liu from Institute of Biomedical Sciences, and came up with a way to apply physical stimulation to test if such mechanical stress to the skin would cause any enhanced inflammation in Blimp-1 lacking mice. As a result, such stimulation proved to have caused the Blimp-1 lacking mice to start the immune responses. The same pattern occurred after topical application of organic compounds to induce dermatitis on their ear skins.
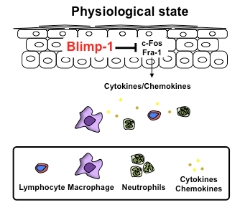
The team concluded by then, lack of Blimp-1 in the skin cells has made the skin immune system much more sensitive, and by a slim outside stimulation, the immune system started to kick off. Further study also revealed that these infiltrating immune cells were neutrophils and macrophages, both are activated during inflammation. It is almost certain that, epidermal Blimp-1 acts like a gatekeeper, which has the role of giving the final “go” command in cases of activation. However, when Blimp-1 is missing, two transcription factors Fos and Fra-1 responsible for the synthesis of cytokines/chemokines took the commanders role and sent out the orders to call to actions of neutrophils and macrophages.
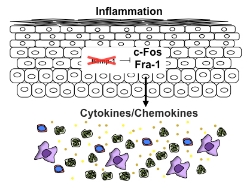 InflammationIn the case that Blimp-1 has been missing for a long period of time, these Fos and Fra-1 acting commanders don’t have any idea of ceasefire, they just keep sending the signals for recruiting more and more neutrophils and macrophages, thereby the skin inflammatory disorders, such as eczema, may occur.
InflammationIn the case that Blimp-1 has been missing for a long period of time, these Fos and Fra-1 acting commanders don’t have any idea of ceasefire, they just keep sending the signals for recruiting more and more neutrophils and macrophages, thereby the skin inflammatory disorders, such as eczema, may occur.
Accordingly to Dr. Lin, many skin diseases may originate from defects in immune responses. They have high hopes that this study would bring more clues to scientists and medical professions to pinpoint the causes for such inflammatory disorders and the ways of corrections.