Breast cancer has been the most common cancer in women worldwide. Even though early detection and therapeutic strategies have made breast cancer less life-threatening and increased the 5-year survival rate to more than 90%, the survival rate is still only 30% for later stage breast cancers that have metastasized. Therefore, better knowledge of how breast cancers spread to other parts of the boy is a key factor to improve survival.
Professor Wendy W. Hwang-Verslues of Genomics Research Center discovered that expression of Desmoglein2 (DSG2), a component of the desmosome complex that enhances adhesion between cells, is strongly correlated with poor prognosis and high recurrence in breast cancer. Based on the oxygen level in the microenvironment, the level of DSG2 expression can dynamically increase and decrease to facilitate different stages of cancer cell release from the primary tumor and colonization of a new site in the body. These findings reveal the importance of DSG2 in all stages of breast cancer metastasis and make DSG2 a good candidate for finding a way to inhibit breast cancer metastasis. This research has been published in the prestigious journal Proceedings of the National Academy of Sciences of the United States of America (PNAS).
 |
| Dr. Wendy W. Hwang-Verslues(right) and first author Dr. Po-Hao Chang(left) |
“Our team analyzed a tumor transcriptome datasets compiled by many researchers. Among the genes associated with metastatic disease, DSG2 was the most highly expressed and this told us that it would be a promising target for detailed study in our laboratory,” said Hwang-Verslues.
The Hwang-Verslues laboratory also used data collected from clinical biopsies as well as three independent breast cancer cohorts in Taiwan. All this information indicated that DSG2 expression may lead to breast cancer metastasis and recurrence.
The Hwang-Verslues team also established two different mouse models to investigate the tumorigenic abilities of DSG2-expressing and DSG2-depleted breast cancer cells. They found that tumors derived from DSG2-expressing cells were larger and generated more circulating tumor cell (CTC) clusters to drive metastasis. CTC are groups of cancer cells that have detached from the primary tumor and circulate in the bloodstream. CTC clusters are the main way that cancer cells can settle in a new organ to form a metastatic tumor.
What impressed us most is that DSG2 expression increased CTC clusters in the blood and also increased tumor growth in the mammary tissue.” Dr. Hwang-Verslues commented. In recent studies, CTC clusters appear to have greater metastatic potential than single CTCs. It is believed that collective movement makes these cancer cells more apoptosisresistant, more capable of avoiding immune surveillance, and easier to colonize in distant organs.
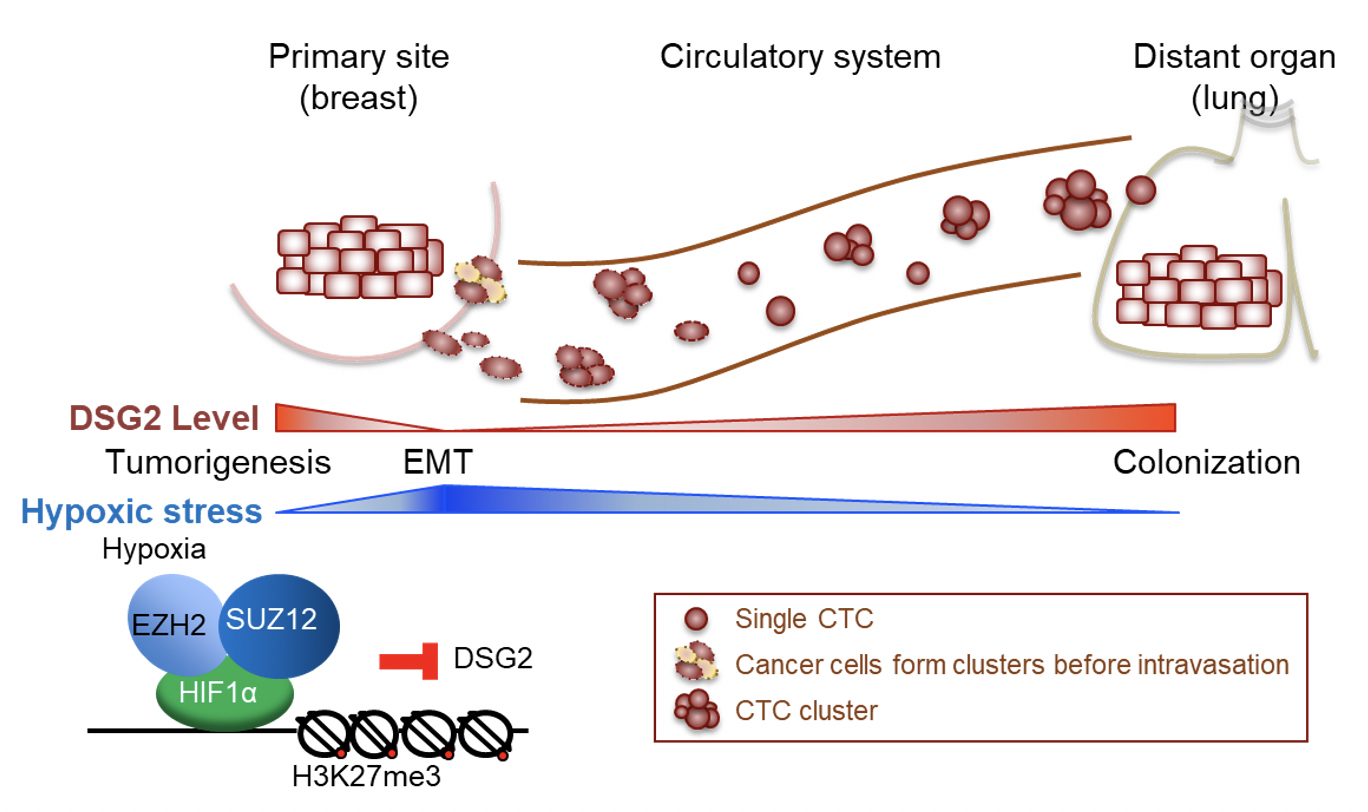 |
| Dynamic changes of DSG2 expression contribute to breast tumorigenesis and metastasis. |
The team was puzzled for a while because high DSG2 means more adhesive strength between cells, so, why there were more runaway tumor cells?
This question led them to discover that as the tumor growth is promoted by DSG2 expression, it rapidly outgrows its blood supply and oxygen is depleted. In hypoxic regions, the key regulatory protein HIF-1α senses the low oxygen level to reduce DSG2 expression. As a result, the cancer cells are less adherent and detach themselves from the primary tumor, and enter the bloodstream. These single CTCs were able to reactivate DSG2 expression once they were inside the bloodstream where oxygen is no longer low. The cancer cells then regain growth and adherence potential that increases their ability to colonize distant organs.
The transcriptional activation function of HIF-1α plays a critical role in metastasis, but it has not been seen to suppress an oncogenic factor to drive cancer progression. “We are the first in the field to report the transcriptional suppression function of HIF-1α on an oncogenic factor in the tumor progression process.” Dr. Hwang-Verslues said.
Based on clinical data and animal models, these researchers demonstrated that DSG2 can be used as a prognostic marker for breast cancer. Interestingly, DSG2 expression is also associated with prognosis in other cancers including cervical, head and neck, and lung cancers. It looks promising in using DSG2 for drug development studies. Using a monoclonal DSG2 specific antibody to target the DSG2 to inhibit anchorage-independent growth may be possible. However, development of therapeutic strategies targeting DSG2 must account for how both high and low DSG2 expression promote different stages of the cancer metastasis process.
The Taiwan Cancer Registry data from 2018 showed that breast cancer is the most common malignancy among women in Taiwan. Professor Wendy W. Hwang-Verslues’s team has taken a big step in understanding breast cancer metastasis.
The complete result of this study can be read online at: https://www.pnas.org/content/118/3/e2014408118